Scientists from The University of Melbourne have developed a world-first vaccine to treat gum disease. Their research, published in the journal NPJ Vaccines, has so far only tested the vaccine in mice.
If successful in human trials, the vaccine will be able to prevent chronic gum disease – or periodontitis – that is considered the main cause of tooth loss in people over 30 years old globally.
What is periodontitis?
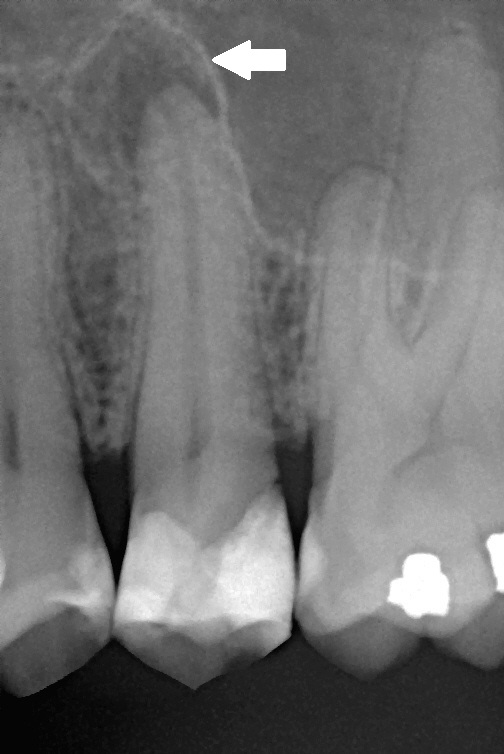
Periodontitis causes irreversible destruction of the bone and gum holding teeth in place. If left untreated, it leads to tooth loss.
Chronic gum disease affects 10 to 15% of the global population on average, although recent studies from the United States suggest up to half the population might be affected, with varying severity.
The prevalence of periodontitis increases with age and around 53% of Australians aged 65 and over have moderate to severe levels.
For most people, the disease progresses slowly over a period of 20 to 30 years, before they start losing teeth. Periodontitis is generally painless until the later stages and many do not know they have problems.
At the start and throughout the disease process, there is commonly bleeding from the gums on brushing and flossing. Some patients report bleeding on eating and overnight.
As the disease progresses teeth may become loose, there may be recurrent swelling of the gums, a bad taste and/or bad breath. Gums can start receding from the tooth, leading to sensitivity to hot, cold and sweet things.
In many cases, it is a visit to the dentist that identifies the problem.
What causes gum disease?
Periodontitis starts with bacteria accumulating around the gum line of the teeth forming plaque. It’s thought the person’s immune response to the bacteria is what does the damage.
The response leads to gums becoming inflamed which causes them to bleed and detach from the tooth forming “pockets”. The plaque then grows into these pockets below the gum level. Once under the gum, brushing and flossing will not remove it.
The initial stage of inflammation due to plaque formation is called gingivitis.
Over time, the pockets increase in depth and the bone around the teeth is destroyed, while the gums recede. Eventually, if left untreated, the tooth will be lost.
Risk factors for getting gum disease include having poor oral hygiene, being a man, low levels of income and education, smoking, diabetes and lack of visits to the dentist.
The inflammatory response initiated by the bacteria seems to affect more than just the gums. Recently, links with heart disease and diabetes have been identified in some patients with periodontitis.
How is it treated?
All dentists are trained to detect gum problems, which reinforces the need for regular dental check-ups. If the disease is severe, patients are generally referred to a gum specialist or periodontist.
Treating gum disease generally involves improving oral hygiene and removing deposits under the gum, as well as removing plaque and calculus (which is when plaque hardens with time) from teeth. This is something a dentist or dental hygienist will do.
Hopeless teeth will often need to be extracted.
Regular three-, four-, or six–monthly follow up is necessary to maintain improvement and, hence, keep teeth.
Management of risk factors is vital. Stopping smoking improves treatment outcomes as does good sugar control in diabetics.
In severe cases that don’t respond well to conventional treatments, antibiotics or gum surgery are often considered. However, the underlying susceptibility to gum disease will always be there and without proper and regular follow up, it recurs with subsequent tooth loss.
In a small proportion of periodontitis patients there is further progression of the disease and tooth loss irrespective of regular care.
How can it be prevented?
Good oral hygiene is paramount to preventing gum disease. Most people clean their teeth with a toothbrush, but also cleaning between teeth is important to help prevent gum problems. This can either be with floss, toothpicks or interdental brushes.
Regular visits to the dentist or dental hygienist for gum assessment and cleaning is necessary. It is much easier to manage the earlier stages of gum disease.
Managing the bacteria that starts the cascade of events leading to periodontitis is key to beating it. This is where the periodontal vaccine fits in with treatment.
Recently, one bacterial species has been singled out as the main pathogen, or culprit. In sufficient numbers, it affects the types of bacteria that build up, as well as the subsequent immune response causing more destruction of the gums.
If this species can be controlled, there should theoretically be much less disease or recurrence of it. The vaccine will stimulate the host’s immune response to produce antibodies towards this species preventing numbers from building up and reducing the inflammatory response and the amount of destruction.
This will result in improved long-term outcomes and make management much easier and less costly.
 Ivan Darby receives funding from NHMRC, ADRF & APRF.
Ivan Darby receives funding from NHMRC, ADRF & APRF.
This article was originally published on The Conversation. Read the original article.



 Weight-Loss Drug Ads Take Over the Super Bowl as Pharma Embraces Direct-to-Consumer Marketing
Weight-Loss Drug Ads Take Over the Super Bowl as Pharma Embraces Direct-to-Consumer Marketing  Sanofi Reports Positive Late-Stage Results for Amlitelimab in Eczema Treatment
Sanofi Reports Positive Late-Stage Results for Amlitelimab in Eczema Treatment  AstraZeneca’s LATIFY Phase III Trial of Ceralasertib Misses Primary Endpoint in Lung Cancer Study
AstraZeneca’s LATIFY Phase III Trial of Ceralasertib Misses Primary Endpoint in Lung Cancer Study  GLP-1 Weight Loss Pills Set to Reshape Food and Fast-Food Industry in 2025
GLP-1 Weight Loss Pills Set to Reshape Food and Fast-Food Industry in 2025  Innovent Biologics Shares Rally on New Eli Lilly Oncology and Immunology Deal
Innovent Biologics Shares Rally on New Eli Lilly Oncology and Immunology Deal  TrumpRx.gov Highlights GLP-1 Drug Discounts but Offers Limited Savings for Most Americans
TrumpRx.gov Highlights GLP-1 Drug Discounts but Offers Limited Savings for Most Americans  Sanofi to Acquire Dynavax in $2.2 Billion Deal to Strengthen Vaccine Portfolio
Sanofi to Acquire Dynavax in $2.2 Billion Deal to Strengthen Vaccine Portfolio  RFK Jr. Overhauls Federal Autism Panel, Sparking Medical Community Backlash
RFK Jr. Overhauls Federal Autism Panel, Sparking Medical Community Backlash  California Jury Awards $40 Million in Johnson & Johnson Talc Cancer Lawsuit
California Jury Awards $40 Million in Johnson & Johnson Talc Cancer Lawsuit  Eli Lilly and Novo Nordisk Battle for India’s Fast-Growing Obesity Drug Market
Eli Lilly and Novo Nordisk Battle for India’s Fast-Growing Obesity Drug Market